NEW YORK | The Andes virus holds a unique and troubling distinction in virology. Among the dozens of known hantavirus strains circulating in rodent populations worldwide, it is the only one documented to spread from person to person. Every other hantavirus kills in isolation, infecting a single human through rodent contact and going no further. The Andes strain can keep going.
That distinction is why the ongoing outbreak aboard the MV Hondius cruise ship has drawn a level of global health scrutiny far beyond what a typical hantavirus case would generate. And it is why understanding the precise mechanics and limits of Andes virus transmission is not just an academic exercise. It is a public health necessity.
This article examines what peer-reviewed research has established about how the Andes virus transmits between humans, what remains scientifically unresolved, and what the 2026 MV Hondius outbreak adds to that body of knowledge.
Background: How Hantaviruses Normally Spread
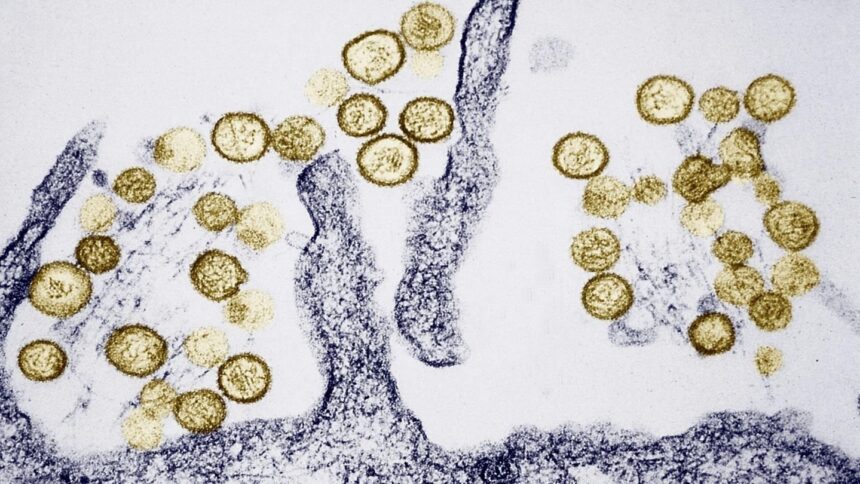
Hantaviruses are RNA viruses carried asymptomatically by specific rodent reservoir hosts. In their natural hosts, the viruses cause persistent infection without harming the animal. Transmission to humans occurs almost exclusively through inhalation of aerosolised particles from infected rodent urine, droppings, or saliva, or through direct contact with those materials followed by mucous membrane exposure.
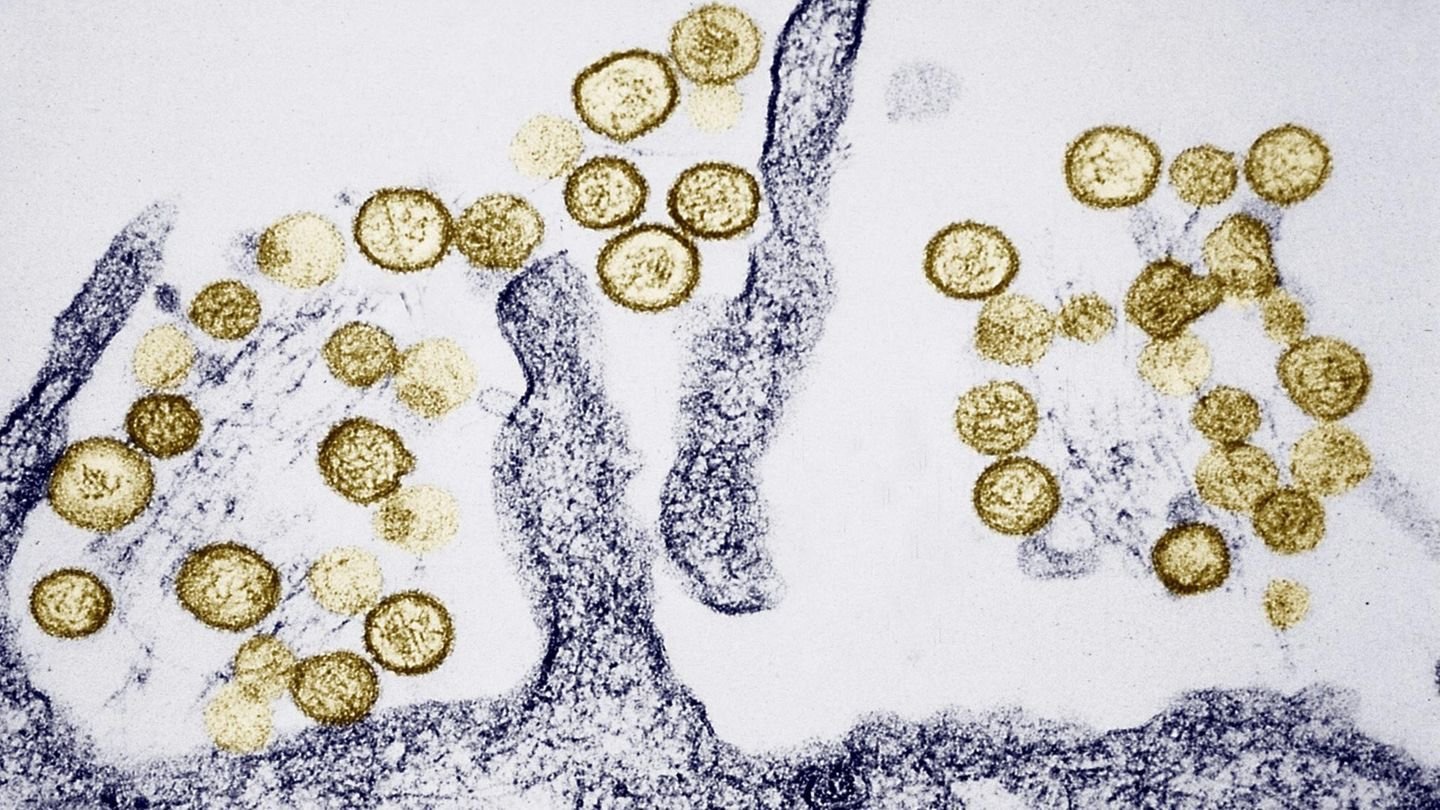 According to the CDC, typical human hantavirus infections are epidemiological dead ends. A person becomes infected through rodent contact, may become severely ill, but does not pass the virus to another person. This pattern holds for all known hantavirus strains with one confirmed exception.
According to the CDC, typical human hantavirus infections are epidemiological dead ends. A person becomes infected through rodent contact, may become severely ill, but does not pass the virus to another person. This pattern holds for all known hantavirus strains with one confirmed exception.
The Andes Virus Exception
The Andes virus is the only hantavirus known to be transmitted from person to person. Human-to-human transmission was first identified during a 1996 outbreak in southern Argentina, and sustained generational transmission was subsequently documented during the 2018 to 2019 Epuyen outbreak.
The Andes virus was first characterized following a 1995 outbreak in the Andean region of Patagonia, Argentina, and since then more than 1,200 cases have been confirmed in Argentina alone.
According to Dr. Gustavo Palacios, a microbiologist at the Icahn School of Medicine at Mount Sinai in New York who helped reconstruct how the virus moved from person to person during the Epuyen outbreak, there have been fewer than approximately 300 documented cases of human-to-human transmission of the Andes virus in history, out of roughly 3,000 total Andes cases overall.
Those numbers put the MV Hondius outbreak into sharp perspective. At eight confirmed or suspected cases across multiple countries as of May 7, 2026, the ship cluster represents a meaningful addition to the global record of documented Andes virus person-to-person transmission events.
The Transmission Window: When the Andes Virus Spreads
Understanding when the Andes virus is transmissible between humans is critical for containment, and this is where the research is most precise.
Transmission primarily occurs among family members or during prolonged close contact with an infected individual in the prodromal phase of the disease. The prodromal phase refers to the early stage of illness, typically characterised by fever, muscle pain, headache, nausea, and vomiting, before the more severe cardiopulmonary symptoms develop.
Epidemiologic and genetic data from multiple cluster studies show that person-to-person spread of the Andes virus likely takes place during the prodromal phase or shortly after it ends.
A 2024 prospective study published in The Lancet Infectious Diseases examined viral shedding patterns in confirmed Andes virus patients. The study found close contact with an infected person during the prodromal phase, specifically activities such as deep kissing, sexual contact, sharing food or drinks, or breastfeeding, was associated with high-risk transmission. The research also found significant viral shedding for up to 16 days after symptom onset, with the virus detected in multiple body fluids including saliva, urine, and nasopharyngeal secretions.
A study of the 2018 Epuyen outbreak found that most human-to-human transmissions occurred on the first day the infected person had a fever, highlighting the importance of early isolation.
The 2018 to 2019 Epuyen Outbreak: The Most Documented Case Study
The Epuyen outbreak in Argentina’s Chubut Province remains the most comprehensively studied instance of sustained Andes virus person-to-person transmission in history. Its findings directly inform the response to the MV Hondius cluster.
On November 2, 2018, a person-to-person transmission outbreak of the Andes virus began in the small town of Epuyen, Argentina. The strain demonstrated a high capacity for sustained transmission among the human population requiring the implementation of quarantine measures, rigorous contact tracing, isolation of close contacts, and active clinical monitoring to prevent further spread.
A phylogenetic analysis confirmed the outbreak was caused by a single spillover event from rodents to humans. Three patients were the main drivers of the outbreak and were the source of 64% of secondary cases, amounting to 21 of 33 total cases. The transmission and exposure events for all 33 secondary cases and four waves of human infection were reconstructed based on known and probable epidemiological relationships. The first person-to-person transmission event was traced to a birthday party with approximately 100 guests.
The index patient attended the party for 90 minutes and was reportedly symptomatic at the time, with fever and malaise. Five persons who had been seated close to the index patient reported onset of symptoms between 17 and 24 days after the party. One secondary case became the source of six additional infections during his early prodromal phase because of his active social life. He died 16 days after symptom onset, and his spouse was febrile while attending his wake. An additional 10 persons who attended the wake and were in close contact with his spouse became ill between 14 and 40 days later.
Dr. Palacios noted that the vast majority of known cases of human-to-human spread of the Andes virus have involved people in close contact relationships, such as those living together, in intimate relationships, or healthcare workers treating sick patients. Fewer than 50 cases have involved more casual contact, including one instance in which a person became sick after a brief conversation with an infected individual.
The key lesson from Epuyen for the MV Hondius response is that isolation of symptomatic individuals during the prodromal phase is the single most effective intervention available. Argentine scientists found that isolation measures helped stave off a wider outbreak in Epuyen.
What the Science Still Does Not Fully Resolve
Despite the Epuyen research, important scientific questions about Andes virus transmission remain open.
While major public health organisations including the CDC recognise person-to-person transmission based on epidemiological clustering and viral genome sequencing, a 2022 systematic review concluded that the existing observational outbreak studies lack the formal environmental control groups required to definitively eliminate the possibility of simultaneous environmental rodent exposure as an alternative explanation in some cases.
In other words: the evidence for person-to-person transmission is strong and broadly accepted, but the precise biological mechanism by which the virus crosses between humans, and the exact dose of exposure required to cause infection, are not fully characterised. No controlled experimental studies in humans are possible for obvious ethical reasons.
Research on the incubation period for Andes virus infection has established a range of 7 to 39 days based on a cohort of 20 patients with well-defined exposure periods. This wide window creates significant challenges for contact tracing and quarantine protocols, since individuals who were exposed may not develop symptoms for more than a month.
What the MV Hondius Outbreak Contributes
The 2026 MV Hondius outbreak is the first documented case of sustained Andes virus transmission in a closed maritime environment, and it presents a set of epidemiological conditions that the Epuyen outbreak did not.
On a cruise ship, passengers share enclosed ventilated spaces, dining areas, and common facilities over an extended period. The index case, a Dutch couple who likely contracted the Andes strain during a birdwatching trip near Ushuaia, Argentina before boarding, would have been in the prodromal phase of illness during the early portion of the voyage. That timing overlaps with the period of peak human-to-human transmissibility identified in the Epuyen research.
As of May 7, 2026, the WHO has confirmed eight cases linked to the ship across multiple countries, with three deaths recorded. The cases span passengers who had varying degrees of contact with the index couple, from close social interactions to more incidental proximity. The epidemiological mapping of exactly who was exposed and when, compared against the transmission window data from Epuyen, will be a critical data set for researchers studying Andes virus behaviour in non-endemic, non-household settings.
The CDC confirmed it is monitoring the situation closely and coordinating with international health partners. Stool specimens and other biological samples have been collected from symptomatic passengers for laboratory analysis.
For full coverage of the MV Hondius outbreak and its global implications read:
- Hantavirus Outbreak on MV Hondius Cruise Ship Sparks Global Concern
- Hantavirus Symptoms 2026: What to Know About Transmission and the Andes Strain
- Pfizer Document Lists Hantavirus Among 1,233 Monitored Conditions
Prevention and Containment Implications
The accumulated research on Andes virus transmission points to a consistent set of conclusions for public health response.
Early symptom recognition and immediate isolation of individuals in the prodromal phase is the highest-impact intervention available. Contact tracing must account for the full 7 to 39 day incubation range. Personal protective equipment including gloves, masks, and eye protection is recommended for healthcare workers and household contacts of confirmed cases during the infectious period. There is currently no licensed vaccine or specific antiviral treatment for Andes virus infection. Treatment remains supportive, with mechanical ventilation required in severe cardiopulmonary cases.
The UK Health Security Agency and European Centre for Disease Prevention and Control have both issued guidance to clinicians advising that any patient presenting with fever, myalgia, and respiratory symptoms following travel to South America or contact with known MV Hondius passengers should be assessed for Andes virus infection.
Conclusion
The Andes virus occupies a genuinely unusual position in the landscape of infectious diseases. It is rare enough that the entire documented history of human-to-human transmission amounts to roughly 300 cases globally. It is dangerous enough to carry a case fatality rate of up to 50% in some outbreak settings. And it is scientifically unresolved enough that researchers are still characterising the precise conditions under which one human infects another.
The 2018 Epuyen outbreak provided the most detailed map of Andes virus transmission dynamics to date. The 2026 MV Hondius outbreak will add a new chapter to that map, one set in a closed international environment with passengers from 23 countries, a long voyage through remote waters, and a delayed recognition of the index case. The data gathered from this outbreak, once fully analysed, will materially advance scientific understanding of how this virus behaves outside its endemic rodent-human spillover context.
That understanding matters. Not because the Andes virus is likely to become a pandemic pathogen, but because the next outbreak, wherever it occurs, will be managed more effectively if the lessons of both Epuyen and the MV Hondius are properly documented and applied.
Peer-Reviewed Sources:
- Martinez VP et al. Person-to-Person Transmission of Andes Virus. Emerging Infectious Diseases. 2005;11(12). CDC/EID
- Vilibic-Cavlek T et al. Super-Spreaders and Person-to-Person Transmission of Andes Virus in Argentina. New England Journal of Medicine. 2020. NEJM
- Viral Shedding and Viraemia of Andes Virus During Acute Hantavirus Infection. The Lancet Infectious Diseases. 2024. ScienceDirect
- Incubation Period of Hantavirus Cardiopulmonary Syndrome. Emerging Infectious Diseases. PubMed Central
- Virological Characterization of ARG-Epuyen Strain. PMC/NCBI. 2026. PubMed Central
- CDC Andes Virus Overview
- WHO Disease Outbreak Notice: MV Hondius 2026
- Andes Virus on Wikipedia