NEW YORK | Most people had never thought twice about hantavirus before the MV Hondius cruise ship outbreak put it on the front page of every major news outlet. Now, with eight confirmed or suspected cases spread across multiple countries and nearly 150 passengers preparing to disembark in Tenerife, millions of people are asking the same basic questions.
What exactly is hantavirus? How does it spread? What does it feel like? And should the average person be worried?
Here is a clear, plain-language breakdown of everything you need to know.
What Is Hantavirus?
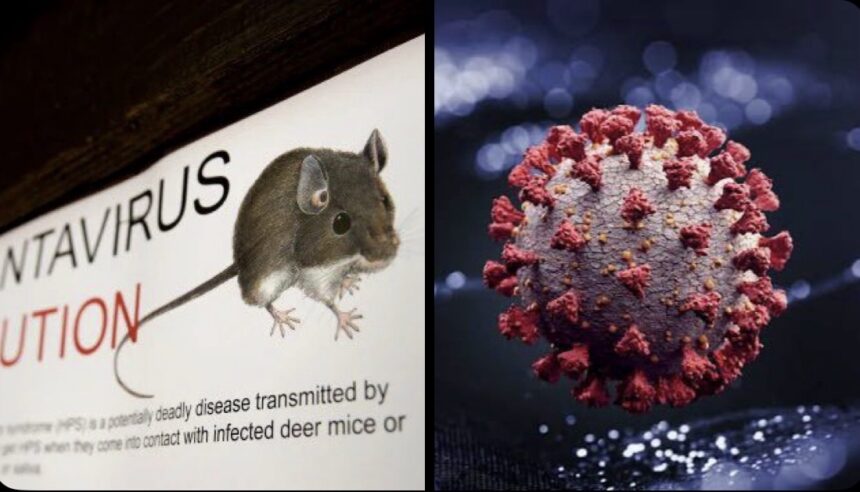
Hantavirus is a family of viruses carried by rodents. The animals themselves do not get sick from it, but they shed the virus through their urine, droppings, and saliva. When people come into contact with those materials, or breathe in particles contaminated by them, infection can follow.
There are dozens of known hantavirus strains around the world. They fall into two broad categories based on the disease they cause in humans. In the Americas, hantaviruses typically cause Hantavirus Pulmonary Syndrome (HPS), a severe respiratory illness. In Europe and Asia, most strains cause Haemorrhagic Fever with Renal Syndrome (HFRS), which primarily attacks the kidneys rather than the lungs.
The strain behind the MV Hondius outbreak is the Andes virus, found in South America and carried mainly by the long-tailed pygmy rice rat. It causes HPS and carries a case fatality rate of up to 40%, making it one of the more dangerous known hantavirus strains.
How Does Hantavirus Spread?
For most hantavirus strains, the answer is simple: through rodents. Specifically through:
- Breathing in contaminated air in enclosed or poorly ventilated spaces where rodents have been active
- Touching surfaces, soil, or objects contaminated with rodent urine, droppings, or saliva and then touching the mouth or eyes
- Being bitten by an infected rodent, though this is rare
- Farming, forestry work, cleaning out sheds or cabins, and sleeping in rodent-infested areas are the most common exposure scenarios
What makes the Andes virus different from every other known hantavirus strain is that it is the only one documented to spread between people. According to the CDC, this human-to-human transmission is rare and typically requires close and prolonged contact, particularly among household members or intimate partners.
Research into the 2018 Epuyen outbreak in Argentina, one of the best-documented Andes virus clusters, found that the window for human transmission appears to be short. People are most infectious around the time they first develop a fever. In that outbreak, transmission occurred after relatively brief proximity in some cases, including contact at a birthday party, though most spread happened within households and among caregivers.
The WHO says human-to-human transmission of the Andes virus appears most likely during the early phase of illness. It does not spread through casual contact the way respiratory viruses like influenza or COVID-19 do.
What Are the Symptoms?
Hantavirus symptoms come in stages, and the early signs are easy to mistake for flu. That is part of what makes it dangerous.
Early stage (days 1 to 5 after symptoms begin):
The first signs are typically fever, extreme fatigue, and muscle aches, particularly in the thighs, hips, and back. Headache is common. Many patients also experience gastrointestinal symptoms including stomach pain, nausea, vomiting, and diarrhea. There is no cough or runny nose at this stage, which can help distinguish it from a typical cold or flu if doctors are looking carefully.
Late stage (days 4 to 10):
This is where hantavirus becomes life-threatening. In patients who develop HPS, the lungs begin to fill with fluid as the body’s immune response goes into overdrive. Coughing and shortness of breath appear suddenly and can escalate to respiratory failure within hours. Some patients go into shock. This stage requires intensive hospital care, often including mechanical ventilation.
According to UC Riverside School of Medicine, the progression from early flu-like symptoms to severe respiratory distress can happen within four to ten days of symptom onset, sometimes faster.
The UK Health Security Agency notes that symptoms typically appear between two and four weeks after exposure, though the incubation period can stretch to 40 days in some cases. The WHO puts the general range at one to eight weeks depending on the strain.
This long incubation window is one of the reasons the MV Hondius outbreak is so complex to manage. Passengers who felt fine when they left the ship may still be within their exposure window.
Is There a Treatment or Vaccine?
No vaccine for hantavirus exists for general use. The CDC confirms there is no specific antiviral treatment currently approved for Andes virus or most other hantavirus strains. A vaccine called Hantavax exists in some countries for certain Old World strains, but it is not available for the Andes virus.
Treatment is supportive, meaning doctors manage the symptoms rather than the virus itself. That includes oxygen therapy, fluids, and mechanical ventilation for severe respiratory cases. Early medical intervention significantly improves survival odds, which is why health authorities everywhere are urging anyone with possible exposure to seek care immediately if symptoms develop.
Several research groups are actively working on Andes virus vaccine platforms, including a team at UC Riverside, but none are available to the public yet.
Who Is at Risk?
For the average person going about daily life in a city or suburb, the risk of hantavirus is extremely low. The virus does not spread through casual contact, food, or water. You cannot catch it by being near someone who has it unless you are in close, prolonged contact during their infectious period.
The people most at risk are those with direct rodent exposure. That includes:
- People who work in or clean out buildings, cabins, barns, or storage spaces where rodents have been present
- Farmers and agricultural workers in regions where hantavirus is endemic
- Outdoor enthusiasts camping or working in areas with high rodent populations, particularly in South America, parts of the US Southwest, and rural Europe and Asia
- People in close contact with a confirmed Andes virus patient during the early stage of their illness
For travelers, the CDC notes that the rodents carrying Andes virus have not been found in the United States. The risk for Americans is primarily linked to travel in South America or, as the MV Hondius case illustrates, expedition travel through remote areas where rodent contact is possible.
How Do You Protect Yourself?
Since there is no vaccine, prevention comes down to avoiding exposure.
If you are in an area with known rodent activity, keep food sealed and stored off the ground, avoid handling or disturbing rodent nests or droppings without proper protective equipment, and ventilate enclosed spaces before entering and cleaning them. The CDC recommends wetting contaminated areas with disinfectant before cleaning rather than sweeping or vacuuming, which can stir particles into the air.
For those who may have been in contact with a confirmed Andes virus patient, the key message from health authorities is to monitor yourself for symptoms and seek medical care promptly if any develop. Do not wait to see if symptoms pass on their own.
Is This the Next Pandemic?
No. Health authorities have been clear and consistent on this point.
WHO Director-General Tedros Adhanom Ghebreyesus confirmed the overall public health risk from this outbreak remains low. The Andes virus does not spread easily between people, has not established any community transmission outside the ship, and lacks the biological characteristics needed to become a widespread pandemic pathogen.
As Time Magazine reported, health officials have explicitly stated this is not another COVID. The Andes virus has been circulating in South America for decades. Argentina alone reported 101 hantavirus cases since June 2025, which is roughly double the prior year’s rate, but that increase reflects environmental and ecological conditions, not a new pandemic strain.
What the MV Hondius outbreak does highlight is how quickly a localized case can become an international concern when it involves travelers from 23 countries. That is a surveillance and coordination challenge, not a sign that the virus itself has changed.
What Should You Do Right Now?
If you were on the MV Hondius or shared a flight with anyone linked to the outbreak, health authorities will contact you directly through contact tracing. Do not wait for symptoms to appear before calling your doctor.
If you have not been anywhere near the ship or its passengers, your risk is negligible. Stay informed, but there is no reason for alarm.
If you develop flu-like symptoms after recent travel to South America or after working in environments with possible rodent exposure, mention that history to your doctor. Early detection is the single most important factor in survival.
For our full coverage of the MV Hondius outbreak and the Pfizer document debate, read: